ACL
Our mission at the UPMC Sports Surgery Clinic is to reduce the rates of ACL re-injury. By providing you and your physio with an accurate depiction of your progress to date, how this compares to other pathological and norm populations, and the areas you need to continue to work on, we aim to make this the last time you have an injury. All the information we collect in the service is used to help us understand what we can do to help reduce the risk of re-injury and then, hopefully, help people to stop it happening in the first place. In order to deliver this service, we have put together a team of highly experienced and motivated Biomechanists, Physiotherapists and Strength and Conditioning coaches and housed them in a 14,000 sqft state of the art facility. We have equipped it with gold standard testing equipment to give you a detailed picture of your rehabilitation, to guide you back towards a safe return to play. To aid in developing the service, our team of postdoc and PhD researchers analyse the data to improve the advice and feedback you are given. We then share our findings with the world through peer reviewed publications and presentations all over the globe.
Contents
What is 3D Biomechanics testing?
3D biomechanics involves the use of motion capture software to track the movement of you joints in space, as well as to analyse the forces applied to your body during movement. We are the only clinic in the world offering full AMTI and VICON Nexus 2 and multi-directional biomechanics testing. These allow us to measure joint relationships, forces, peak torques and angular velocities in high-speed cutting, jumping, and landing for both diagnostics, performance, and rehabilitation.
Why do we use 3D Biomechanics testing?
3D motion analysis allows us to analyse your movement in an environment that closely replicates the demands of your sport with a high degree of accuracy in our Astro-turf motion capture laboratory. Your results will be used to accurately tailor your rehabilitation to enhance your functional stability, reduce the risk of future injury and facilitate safe expediated return to performance.
What are the tests?
3D Biomechanics
You will perform a series of double and single leg jumps to assess your explosive and reactive strength. We use force plates to calculate how high you jump, the speed of your jump and the force you produce, whether you are favouring one leg or another, or if there are differences between legs. This will help to inform us of what elements to include in your rehabilitation.
Jump Profiling
Countermovement jump
This test is a measure of jump height and explosive lower limb power which will be performed in double and single leg variations, with symmetry between limbs being an ideal outcome.
Drop jump
This test will measure your plyometric ability and reactive strength – a key quality in injury prevention by ensuring efficient transfer of forces across the hip and groin region during running, jumping and change of direction movements. Like the countermovement jump, this will measure jump height and explosive lower limb power in both double and single leg exercise variations. Single leg variations will only be assessed in your T2 appointment.
Cutting Manoeuvres (T2 only)
90° planned and unplanned cuts
This test replicates hi-speed, sports-specific movements and we will use this to look at your change of direction technique and point out any areas that you may need to work on.
Running Assessment (T2 only)
The aim of this test is to assess your running pattern, as well as the movement of your trunk and pelvis during submaximal running.
Isokinetic strength testing
We use this test to assess the strength of your quadriceps and hamstring muscles over a large range of motion. After your ACL surgery, it is important to ensure any differences in the strength of your thigh muscles is less than 10%.
Testing preparation
To create the 3D model of your body, our technology uses retroreflective markers to reflect infrared light back into our hi-speed cameras. The cameras locate these markers in space and transmit live feedback of your body to our computers. This visual feedback is combined with force data from our force plates to provide a holistic picture of how you move. These markers will be applied to your body using a spray-on plaster and a special double-sided tape. If you have an allergy to plasters, please tell a biomechanist so that suitable adaptations can be made.
This is what you see:
Figure 1.
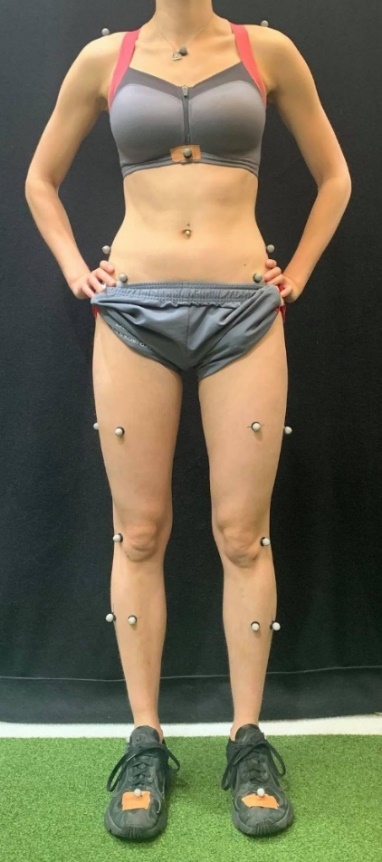
This is what we see:
Figure 2.
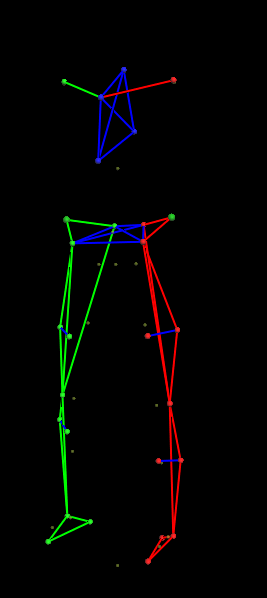
Disclaimer: What we see on the computer is what you see in the follow-up and how we might present data in research. We do not take live video recordings of you, or recordings which may lead to your identification. The only imaging we record is of the 3D stick figure, personalised by only your de-identified patient number and various anthropometric measurements (i.e. height, weight, knee width). This ensures that our data remains anonymous, from data collection to publication. Suitable adjustments can be made for those who have concerns about Figure 1.
T1 at 4 months
You will have your first 3D biomechanical assessment with us at approximately 4 months post-surgery. During this appointment you will be performing the 3D jump profiling and the isokinetic strength assessment.
T2 at 7 months
The final 3D assessment identifies any remaining strength, power or biomechanical deficits that may lead to pain or re-injury when your training load increases or limit your ability to return to optimum performance. During this appointment, you will complete the full testing battery detailed above.
Handing over
After you have completed the testing battery, a follow-up clinician will take you through the 3D motion capture clips alongside a performance report that presents the metrics collected during your assessment. These results contribute to the creation of a comprehensive rehabilitation program going forward, to help speed up return to play times.
How do I prepare?
Please arrive 15 minutes before your appointment is due to start and be ready in appropriate clothing.
Appropriate clothing:
Shorts (ensure they are loose enough to be rolled up)
Ankle socks
Sports bra
Trainers
Extra items:
Towel
Water bottle
Inhaler (if necessary)
If you have long hair, please come with your hair tied back so we can see the top of your neck. Please avoid moisturising or applying tanning products for at least a day before your appointment.
Research and my data
You are playing a huge part in improving outcomes from injury as many have done before you. As with any specific research, full ethical approval was given by the UPMC Sports Surgery Clinic ethics board. This means the research team considered the risks, implications, and validity of the interventions and the data collected. When you enter the service, you will be taken through the testing process, risks and be offered the opportunity to ask any questions. You will then be asked whether you consent to your data being included in our research. This means your de-identified questionnaires, operative notes and biomechanical data will be used for research to further understand ACL injuries. Of course, your participation in the study is entirely voluntary. If you do not wish to participate in the study your decision will not in any way affect your medical care and you can still take part in testing. If you do decide to participate in the study, your identification will remain completely anonymous, and nobody will be able to link the information to you. If you are under the age of 18, a parent or guardian needs to give their consent for your data to be used in research. However, if you the participant do not consent to the use of your data, then it cannot be used in research.










